
Two people sitting together, one resting their head on the other's shoulder in a moment of quiet comfort and support.
The hardest part of the day for many trauma survivors isn't waking life. It's falling asleep.
Nightmares are one of the most common and debilitating symptoms of post-traumatic stress disorder. Unlike the unsettling but random bad dreams most people experience occasionally, PTSD-related nightmares are vivid, repetitive, and often exact replays of traumatic events. They don't feel like dreams. They feel like it's happening again.
More Than a Bad Dream
The scale of the problem is significant. Research published in the Archives of Trauma Research found that up to 71% of trauma victims diagnosed with PTSD experience frequent nightmares, compared to only 2 to 5% of the general population. A 2023 review in Psychiatric Annals put the broader figure even higher, concluding that "upwards of 90% of those with the disorder endorse some form of sleep problem," with insomnia affecting 80 to 90% of patients.
In military populations, the picture is particularly stark. Among active-duty service members and veterans with PTSD, nightmares occur an average of 4.7 times per week (So, Miller & Gehrman, Psychiatric Annals, 2023).

A memorial tribute at the Vietnam Veterans Memorial Wall. Among combat veterans, nightmares are among the most persistent and debilitating symptoms of PTSD.
The distinction between a regular nightmare and a trauma nightmare matters clinically. Standard nightmares occur during REM sleep and typically involve threatening scenarios. They're distressing, but they fade. PTSD nightmares are physiologically more intense, more likely to cause full awakening, and the distress often lingers long after waking. For many survivors, the fear of having a nightmare becomes its own source of anxiety, creating a cycle where dreading sleep makes sleep worse.
What's Happening in the Brain
To understand why PTSD nightmares are so persistent, it helps to understand what's happening neurologically during sleep.
In healthy REM sleep, the brain consolidates memories and processes emotional experiences. Matthew Walker, Professor of Neuroscience and Psychology at UC Berkeley, describes it as a form of "overnight therapy." In a 2011 paper in Current Biology, Walker wrote: "The dream stage of sleep, based on its unique neurochemical composition, provides us with a form of overnight therapy, a soothing balm that removes the sharp edges from the prior day's emotional experiences."
The mechanism involves norepinephrine, a brain chemical associated with stress. In healthy individuals, norepinephrine levels fall significantly during REM sleep, creating a low-stress neurochemical environment in which emotional memories can be reprocessed and softened. For trauma survivors, this process breaks down.
Research from Virginia Tech, published in the Journal of Neuroscience in 2023, showed that in PTSD, neurotransmitter levels remain elevated during REM sleep. As lead researcher Sujith Vijayan explained: "With PTSD, neurotransmitter levels stay high during REM sleep... brain rhythms typically effective in healthy individuals can no longer inhibit fear memories."
The result is that the amygdala, the brain's threat-detection center, remains hyperactivated even during sleep. A comprehensive review in Nature and Science of Sleep (El-Solh, 2018) described the process: "A prolonged hyperactivity of the amygdala may increase the generation of nightmares and alter neural activity in the brain stem and forebrain sleep-regulating centers. The amygdala plays a key role in the processing of fear consolidation, fear extinction, and emotional distress, processes that underlie nightmare generation."
In other words, instead of emotional memories being processed and softened, they're replayed at full intensity. The prefrontal cortex, which normally modulates fear responses, is less active during REM, leaving the amygdala essentially unchecked.
The Physiological Signature
What makes PTSD nightmares detectable, and potentially interruptible, is that they leave a measurable physiological footprint before they fully manifest.
Research published in Psychological Medicine (Mäder et al., 2021) found that elevated heart rate response to stimuli during sleep significantly predicted both PTSD diagnosis and the presence of posttraumatic nightmares. A separate study in Sleep (Nielsen et al., 2010) found that nightmare sufferers show distinct heart rate variability patterns during REM: higher sympathetic activity and reduced parasympathetic tone, alongside measurably longer REM latencies compared to non-nightmare sleepers.
These are the signals that tools like SleepSafe monitor. Heart rate begins climbing before the nightmare reaches its peak. Micro-movements increase. In some cases, breathing patterns shift. This opens a narrow window for intervention before the nightmare fully takes hold.
"The timing is everything," explains Oliver Hebnes, founder of SleepSafe. "Too early and you're interrupting normal REM. Too late and the nightmare has already started. The goal is that narrow window in between."
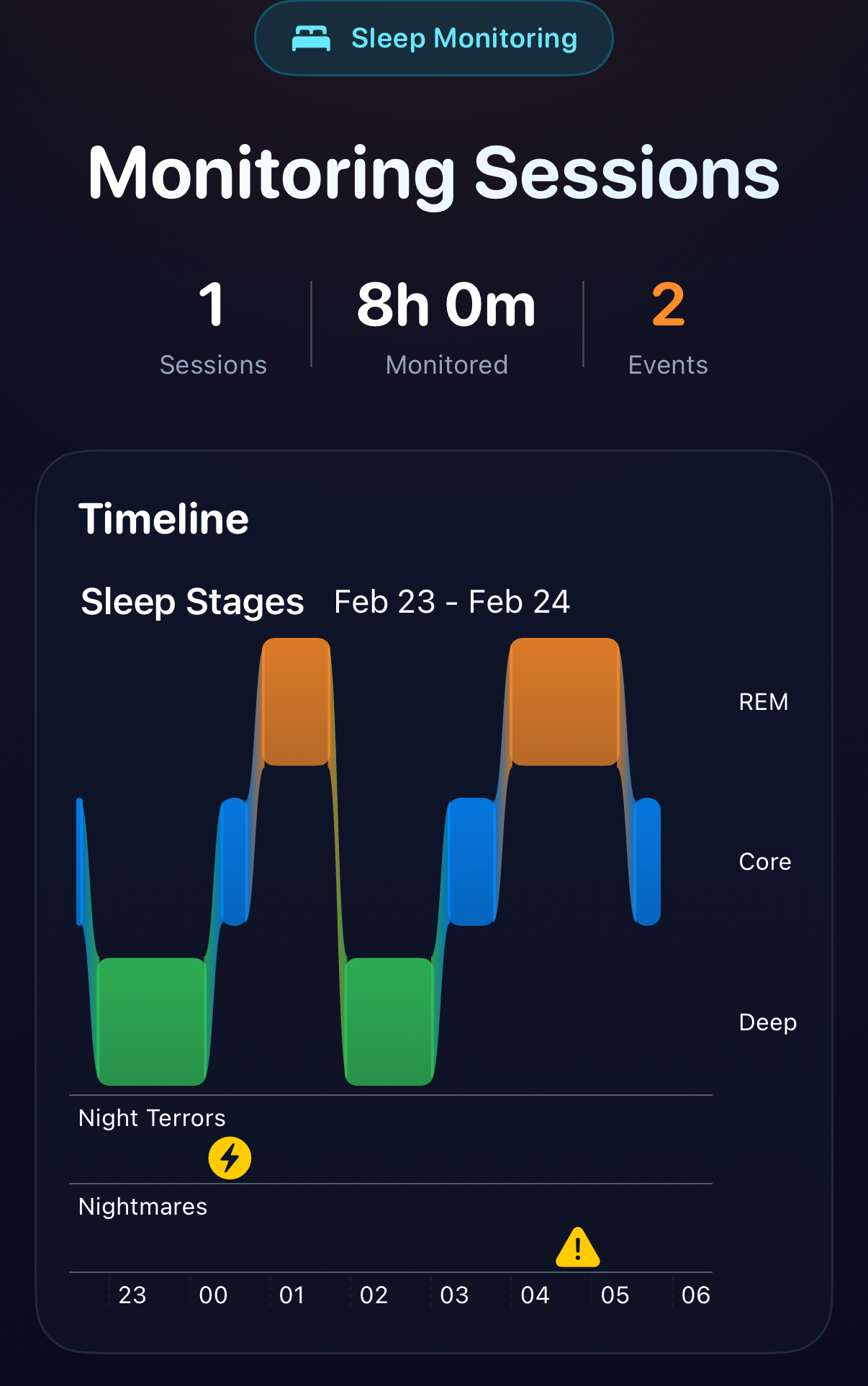
1 session, 8 hours monitored, 2 events detected: a night terror and a nightmare
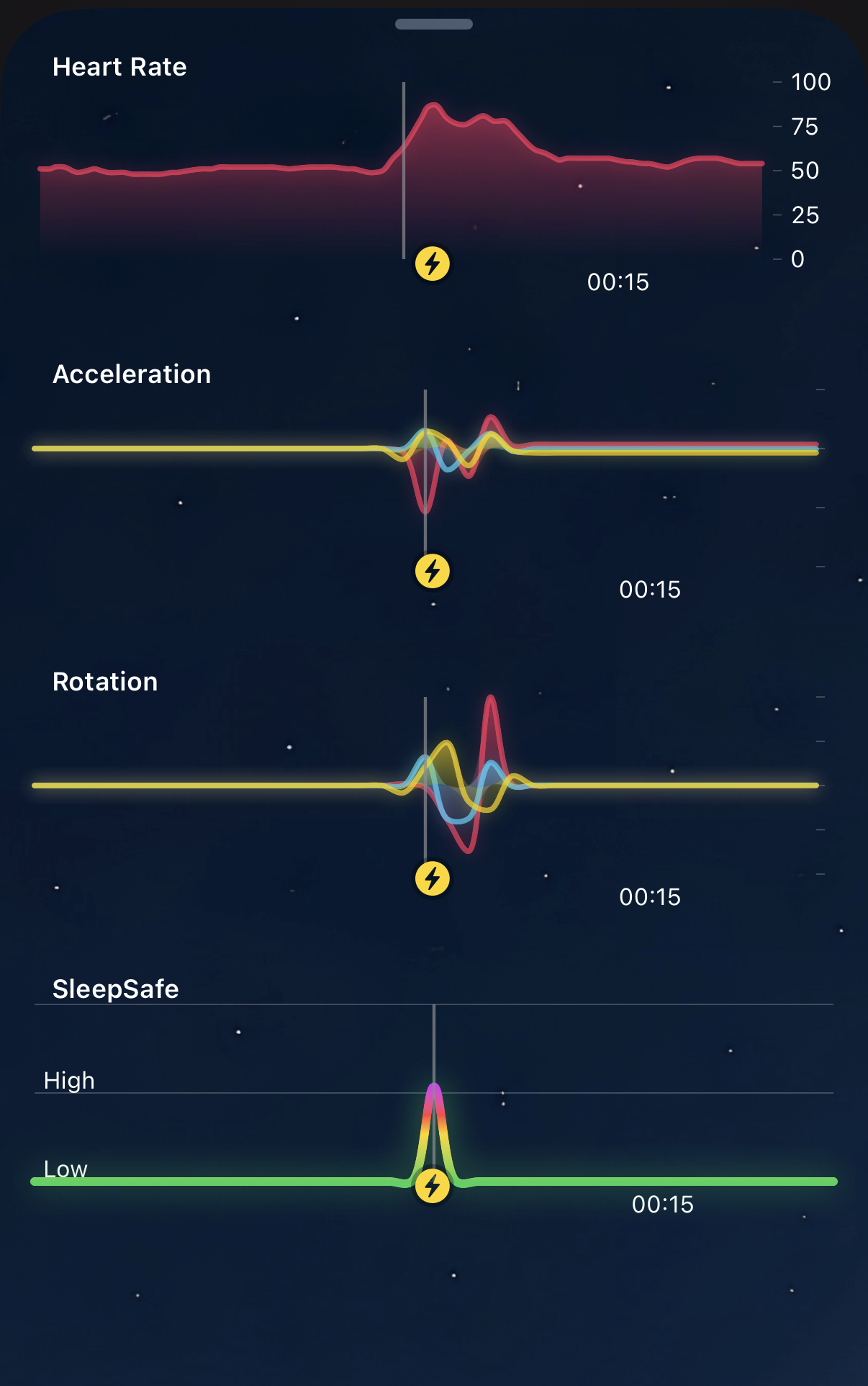
The physiological signature of a night terror: heart rate, acceleration, rotation, and the SleepSafe risk score spiking together. The user did not wake up.
A notable additional finding: unlike typical dreams, which occur almost exclusively in REM sleep, post-traumatic nightmares can arise in both REM and non-REM sleep, a distinction confirmed by ambulatory polysomnography research published in Sleep in 2018.
Sleep As Part of Trauma Recovery
The relationship between sleep and PTSD is not simply that trauma causes bad sleep. Research has established that the two are bidirectionally linked, and that poor sleep can actively block recovery.
Edward Pace-Schott, Anne Germain, and Mohammed Milad, in a 2015 paper in Biology of Mood and Anxiety Disorders, wrote: "Prospective, longitudinal studies have established that sleep disturbances represent a risk factor for the development and course of PTSD, suggesting that sleep is an important neurobiological mechanism in the etiology and maintenance of this disorder." Their research further showed that sleep disruption impairs the brain's ability to consolidate fear extinction memories, undermining the very circuits needed to therapeutically process trauma.
A longitudinal study of U.S. military veterans published in the Journal of Psychiatric Research (2021) found that poor sleep quality was associated with a 60% greater likelihood of developing PTSD. Among veterans who later developed PTSD, 47.8% had reported poor sleep quality at baseline, more than double the 20.7% rate in those who did not go on to develop the disorder.
The clinical implications are significant. Anne Germain, PhD, Director of the Sleep and Behavioral Neuroscience Center at the University of Pittsburgh, has argued that targeting sleep is not just beneficial but potentially essential: "Clinicians need to consider that the chronic sleep disruption associated with nightmares may affect the efficacy of first-line PTSD treatments, and targeted sleep treatments may accelerate recovery from PTSD."
What the Evidence Says Can Help
If sleep disturbance can block PTSD recovery, the question is what can be done about it. Several approaches have meaningful clinical evidence behind them.
Image Rehearsal Therapy (IRT) is the most rigorously studied. The landmark trial, published in JAMA in 2001, randomized 168 sexual assault survivors with PTSD to IRT or a wait-list control. Over three sessions, participants learned to rewrite their nightmare narratives during waking hours. At three-month follow-up, 65% of the treatment group showed at least one level of improvement in PTSD clinical severity. A subsequent meta-analysis by Casement and Swanson, published in Clinical Psychology Review (2012), reviewed 13 studies and 511 participants, finding large effect sizes for nightmare frequency (ES = 0.69), sleep quality (ES = 0.68), and PTSD symptoms (ES = 0.72), with effects holding or strengthening at 6 to 12 month follow-up.
IRT is currently the only Level A recommended treatment for nightmare disorder based on randomized controlled trial evidence.
Prazosin, a medication originally developed for blood pressure, has shown benefit for PTSD nightmares in some patients, though a large VA trial published in the New England Journal of Medicine (Raskind et al., 2018) found mixed results, suggesting that responses vary by subtype.
Technology-assisted monitoring is an emerging complement to these approaches. By detecting physiological signals of nightmare onset and delivering a gentle haptic intervention, tools like SleepSafe aim to interrupt the nightmare cycle at its earliest detectable stage, without full awakening. Several SleepSafe users report having been recommended the app by their therapists as part of a broader treatment plan.
"I'd been in therapy for years," wrote one user. "The daytime stuff was manageable. But every morning I woke up exhausted and shaken, and that affected everything. Using SleepSafe didn't fix the PTSD. Nothing does overnight. But it gave me some nights back."
A Note on Asking for Help
PTSD and trauma-related nightmares carry stigma that can make them hard to talk about. Many people spend years assuming their experience is unusual, or that nothing can be done. Neither is true.
If nightmares are affecting your sleep and your daily life, that is a medical issue, and one that clinicians take seriously. Pace-Schott and colleagues concluded their research with a note of genuine optimism: "Optimizing sleep quality following trauma, and even strategically timing sleep to strengthen extinction memories therapeutically instantiated during exposure therapy, may allow sleep itself to be recruited in the treatment of PTSD."
You don't have to wait until things are unbearable to reach out.
If you experience chronic nightmares or symptoms consistent with PTSD, speak with a healthcare provider or mental health professional. SleepSafe is designed as a complementary tool and is not a replacement for professional treatment.